In many people, the nails and skin are affected by the fungus and do not look pretty. It is important to understand that this is not only an aesthetic issue, but primarily a medical issue.
In some cases, fungal skin damage can be a harbinger of serious conditions such as diabetes. Do not start the disease, as the course of treatment takes on average a year or more.
How can you get skin and nail fungus?
More than 40 parasitic fungi (dermatophytes) are known to affect the skin and nails. The most common are representatives of the genera Trichophyton, Microsporum and Epidermophyton. To grow and reproduce, they use a special matrix called keratin, which consists of the upper layer of the skin (the epidermis), hair and nails. Penetrates the epidermis or nail plate, where the fungus settles and begins to grow and multiply.
If you like to walk barefoot in nature, you can get sick from objects (towels, wooden shelves in bathhouses, saunas, carpets, benches in public swimming pools, manicure/pedicure tools) and contact with soil.
high-risk groups
The most common types of fungal diseases include foot dermatomycosis and nail plate onychomycosis. It takes weeks to months from the moment of infection to the first clinical symptoms.
Men suffer from fungal diseases more often than others. Among women, those who regularly wear pointed shoes, especially high heels, are more likely to develop the disease. In this condition, the toes are constantly squashed, which can lead to friction, small cuts, abrasions, which are all entry points for infection.
You can also "catch" the fungus in a regular salon during a pedicure if the owner uses improperly processed tools. To remove spores and fungal debris from the metal surfaces of forceps, scissors, and tweezers, these tools must be sterilized in a dry heat cabinet. Not all salons have such equipment, so they are limited to "soaking" in sanitizer and "drying" in a UV cabinet. This treatment does not completely prevent infection.
Frequent fungal infections may herald the development of diabetes. According to statistics, diabetic patients are three times more likely to suffer from fungal diseases than diabetic patients. The fungus can also appear allergic skin lesions (itching, inflammation, weeping), grooming insect bites, while taking antibiotics, corticosteroids, antidepressants.
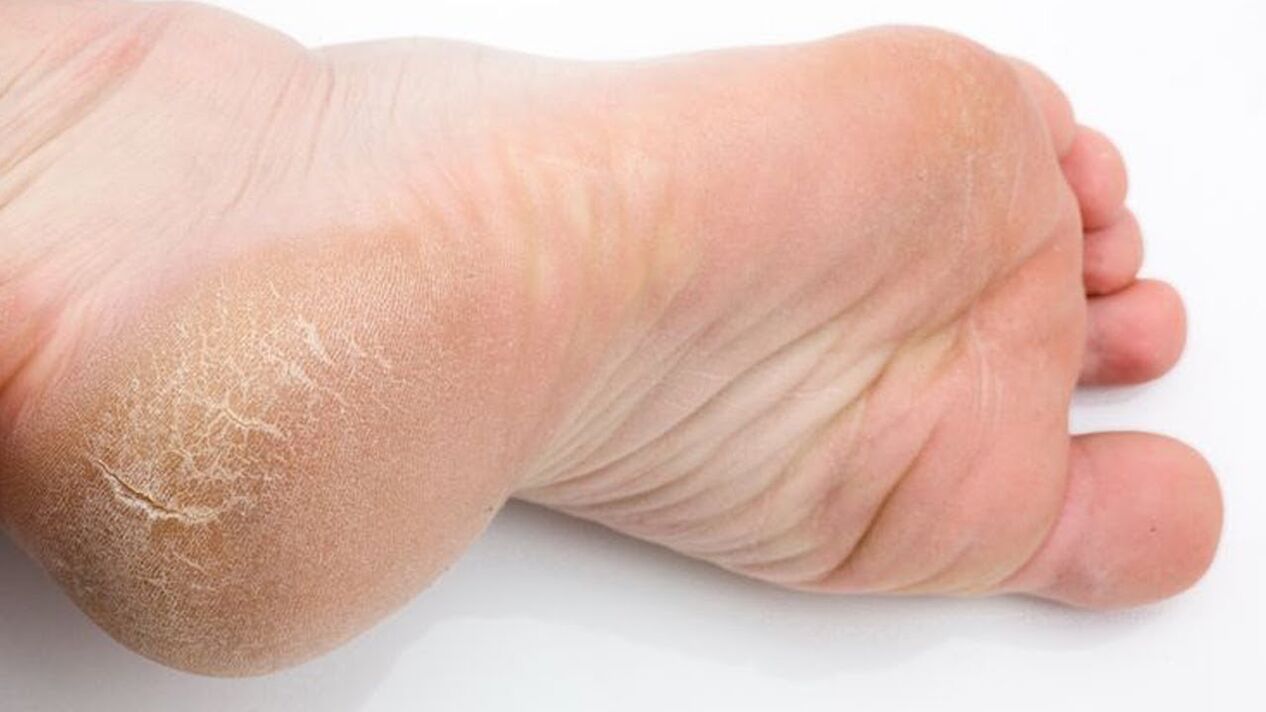
Symptoms of athlete's foot
- Dry skin, cracks, peeling in interdigital folds.
- itching.
- Hyperkeratosis (thickening of the skin on the feet).
- Lesions expand.
- In some cases, a staph infection can appear alongside a fungal infection, which is difficult to cure.
Symptoms of Onychomycosis (Nail Fungus)
Onychomycosis accounts for 40% of all nail diseases. Dermatophytes account for 90% of all nail fungal infections. The most common pathogens are fungi of the genus Trichophyton.
In this case, the appearance of the fungus may be due to an injury to the nail due to high humidity or the constant softening of the nail plate. This is possible, for example, when wearing the same pair of shoes/sneakers every day.
As the infection progresses, the color of the nail changes—parts of the nail turn yellow, gray, or white. Over time, the spots become larger and the nails themselves thicken - subungual hyperkeratosis occurs.
Diagnosis of fungal diseases
For the diagnosis of fungal infections and onychomycosis, special tests that detect fungi are used. Analyze biological material (hair fragments, nail plates, skin particles) under the microscope. The diagnosis is confirmed if infection has occurred and lines of the mycelium (the main body of the fungus) are visible.
If microscopic examination gives an unclear answer, bacteriological examination is carried out - the material is sown on the fungus. The test not only identifies infections, but also susceptibility to antifungal drugs, which is necessary for the selection of effective treatments.
How to protect yourself from fungus
- Dry your feet after bathing or showering, especially between your toes.
- If you wear closed shoes, change your socks daily.
- Change your shoes every two or three days, don't wear the same pair every day.
- Do not walk barefoot in public places (swimming pools, baths, saunas, fitness clubs).
- If someone in your household has fungal disease, provide him with a separate set of towels and sheets. Wash separately at the highest temperature.
- If you have fungus on the same foot or nail, use two different manicure/pedicure sets to avoid spreading the infection to healthy areas.
- If you have diabetes, keep your blood sugar levels under control. "High sugar" slows the healing of skin wounds ("diabetic foot"), which promotes fungal infections.
healthy!
















