One-fifth of the European population suffers from leg fungal disease. These are data from research conducted in all European countries. The most common type of fungus on the feet is the finger folds. The causes are as follows:
These are data from research conducted in all European countries. The most common type of fungus on the feet is the finger folds. The causes are as follows:
- Leg vascular disease (21%);
- Obesity (17%);
- Leg lesions-stenosis between fingers, diabetic feet, flat feet (15%);
- Wearing tight shoes, sports injuries, and pedicure cause skin, nails and fingers injuries.
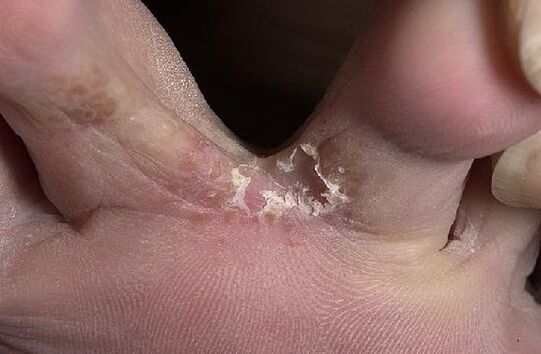
The place where leg fungus is most likely to occur-the tightest space between -3, 4, and 5 toes. From there, the fungus affects all interdigital folds, the skin and side edges of the soles of the feet, the back of the feet, and the nails
How to recognize mycosis of the feet? Toe fungus symptoms
- Cracks or funnels appear between the toes, and the edges of the toes are covered with whitish or greenish scaly (flaky) skin;
- Exudates may leak from the cracks;
- Round diaper rash under and between fingers, peeling skin (trigeminal symptom);
- The airflow between the toes disappeared, and cracks were almost invisible, but the peeling took on a floury characteristic (the skin looks as if it is dusted with flour, which are the affected scales). Symptoms are especially common in children;
- There is a slight itching between the fingers, but there is no great discomfort.
In the "dormant" state, the fungus between the toes will remain indefinitely, thus masking the symptoms. But the process will grow. Gradually, the skin looks more and more dry, rough, rough, and flaky, acquiring a dirty yellow-gray color, keratinized into calcification, and cracks appear especially in rough areas.
Simultaneous or successive stages of onychomycosis-discoloration, thickening, peeling and chipping of nail lesions. When symptoms clearly indicate long-term neglect of health, they achieve this effect in the later stages.
The second path of fungus development between the fingers is relatively rare (about 8%). This is a "wet" vesicle or exudative fungus with ruptured vesicles and ulcers. This wet mycosis between the toes can affect people with severe stress, such as long-term hiking, poorly worn, tight, unventilated shoes, improper fungal treatment, anti-mycotic and glucocorticoid self-treatment.
If the treatment of fungus between the toes is disrupted, 80-100% of patients will be affected by the toenails, and 20% of patients will be affected by the hands. The appearance is sad and offensive, and the nails look like broken dust or laundry soap. It can also take on the appearance of a "vulture claw" or grow into it. Ingrown toenails are also a painful treatment.
How to treat fungus between fingers?
Even if all these symptoms appear many years later, you still need to start treating the fungus between the fingers immediately because it is a highly contagious and stubborn infection.
Let's go to the dermatologist. Before treatment, he scratched with his fingers and checked it using a microscope, culture or DNA analysis. Microscopic examination revealed hyphae or spores.
Systemic treatment involves taking tablets or capsules of antifungal drugs. Those will accumulate in the keratinous tissue within a few weeks after the drug is absorbed, and enter and destroy the fungus through the blood.
The disadvantage is that systemic drugs have moderate hepatotoxicity (they have an adverse effect on weak liver), so this therapy cannot be applied to patients with liver disease, pregnant women, breastfeeding women, and young and old people. The type of drug depends on the nature of the pathogen. If the symptoms are unclear and the type is unclear, a broad-spectrum medication should be prescribed. The use of systemic drugs still has risks; in the advanced stages, long-term treatment is required.
You can also use topical medications that are suitable for the disease. Such drugs usually have a wide range of effects and can kill fungi and bacteria. Treatment is long and intensive, so if funds are limited, you should tell your doctor immediately.
Home remedies and prevention of fungal infections. It is useless to treat the fungus yourself. The information allows us to talk about its excellent survivability and high potential for recurrence.
Prevention is an effective remedy.
- Check for fungal symptoms in family members. Contamination within the family is common. All need treatment;
- Don't use other people's shoes, socks, pedicure equipment, and don't wipe yourself with ordinary towels;
- Not all fungi die even at 100 degrees Celsius, but a large part-yes, so it is feasible to wash bedding and bath towels at 90 degrees.
- Disinfect shoes with antimycotic spray once a month, and disinfect the bathroom surface once a week;
- Do not walk barefoot in public places and perform pedicures in a well-disinfected salon;
- To prevent fungus, you can use anti-fungal ointment, which can clean and dry your feet;
- Do not wear shoes until your feet are dry.
Dermatologists also recommend a pedicure at least half a month every month to remove dead tissue. Fungi like to settle in them. Beware of treatment later.
In the clinic, you can receive examination and consultation from a dermatologist.
















